 
First trimester combined screening will not be reliable if the crown-rump length is greater than 84 mm. Sometimes, it may not be possible to measure NT because of fetal size or technical factors such as fetal position or increased maternal wall thickness. A large prospective NIH study of 38,167 first trimester fetuses reported 117 cases of Down syndrome (0.31 percent)(Malone, 2005).įirst trimester combined screening is reported to have a detection rate for Down syndrome as noted: 87 percent (11 weeks), 85 percent (12 weeks), and 82 percent (13 weeks) at a false-positive rate of 5 percent. This age range corresponds to a fetal crown-rump length between 38 mm to 84 mm. A combined first trimester screening (“FIRST screen”) is currently preferred at our facility and performed between 11 and 13 6/7 weeks gestation. These strategies include the use of combined first trimester screening (NT, PAPP-A, beta HCG only), stepwise sequential (first trimester and second trimester quad screen testing with separate risk estimates given after each test), and fully integrated screening (first trimester NT + PAPP-A + beta HCG with second trimester quad screen where only one risk estimate is given after the quad screen results are available between 15-18 weeks).Īs one option, patients can review their choice of specific genetic tests with our prenatal genetic counselors at the Texas Children’s Pavilion for Women. Several improved tests are based on information from the first trimester to estimate the fetal risk of abnormal chromosomes (e.g. The quad screen detects 81 percent of fetuses with Down syndrome at a 5 percent false-positive rate (Malone, 2005). alpha feto-protein, total human chorionic gonadotropin, unconjugated estriol, and inhibin A) to estimate the fetal risk of Down syndrome. In the late 1980s, obstetricians had once relied on a second trimester quadruple or “quad” screen (15-22 weeks) that combined maternal age with serum markers from the mother (e.g. If prenatal diagnosis was limited to only women greater than 35 years old, only 25-30 percent of chromosome anomalies would be detected. Maternal age alone is not a good screening tool for identifying fetuses at risk for an abnormal number of chromosomes (i.e. beta-human chorionic gonadotropin or b-HCG and pregnancy-associated plasma protein A or PAPP-A). 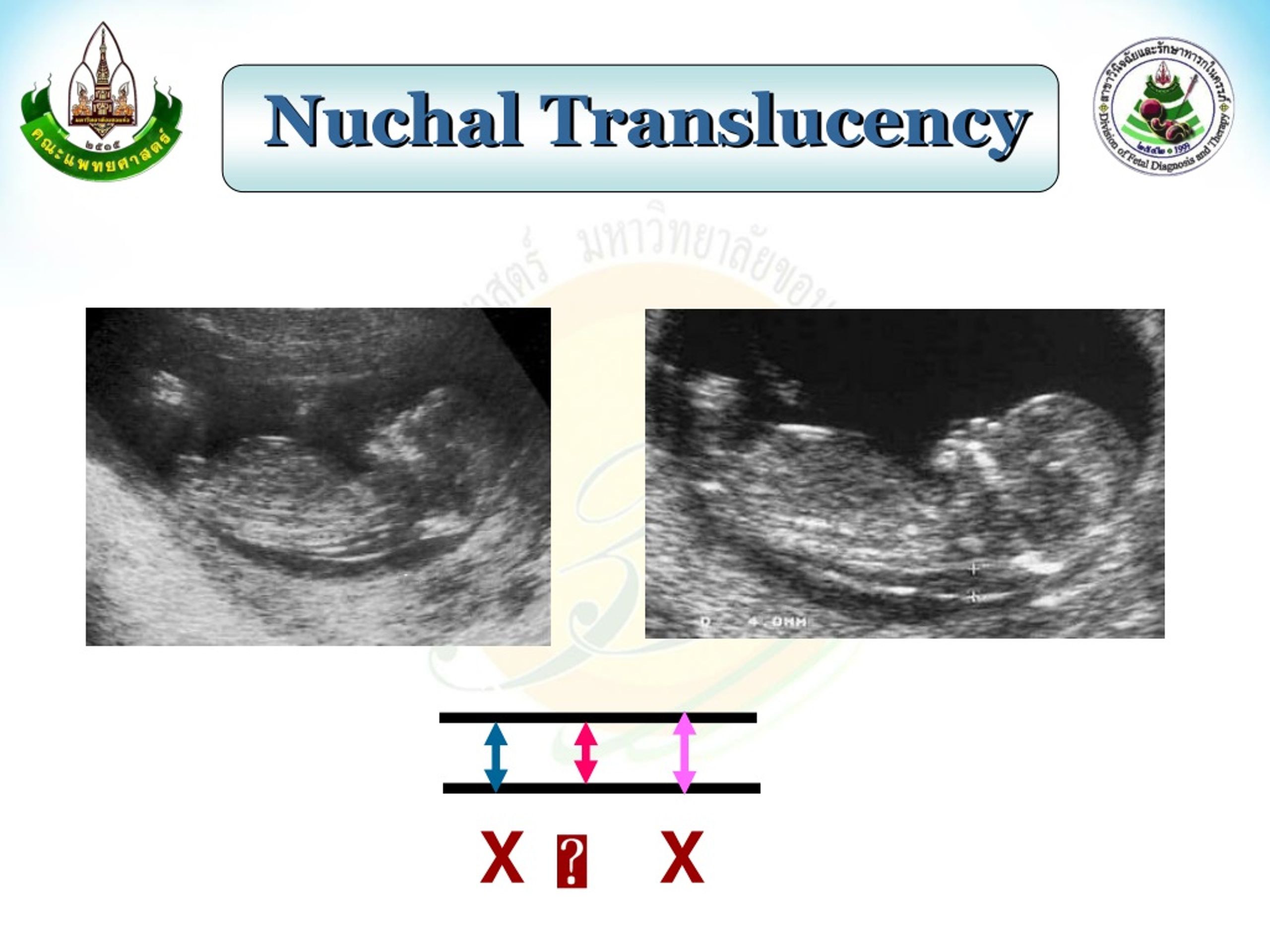
The sensitivity of this screening test can be improved by combining NT results to independent risk estimates by measuring biochemical markers in the maternal circulation (i.e. 
As a single marker, increased nuchal translucency (NT) detected 76.8 percent of fetuses with Down syndrome during the first trimester, although 4.2 percent of the results were falsely positive (Nicolaides, 2004). increased nuchal translucency) is a well-established finding in fetuses with Down syndrome during the first trimester of pregnancy. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
